Hard skills include risk assessment, claims processing, and policy analysis. These are essential for insurance agents to serve their clients well.
Popular Insurance Agent Resume Examples
Check out our top insurance agent resume examples that emphasize essential skills such as client relations, sales strategies, and policy expertise. These examples will guide you in showcasing your strengths to potential employers.
Ready to build an impressive resume? Our Resume Builder offers customizable templates designed specifically for insurance professionals, helping you make a strong impact in your job applications.
Recommended
Entry-level insurance agent resume
This entry-level resume for an insurance agent highlights the applicant's proven sales skills and client relationship management abilities. It showcases significant achievements like increasing policy sales and improving client satisfaction. New professionals in this field should convey their adaptability and results-driven mindset through quantifiable accomplishments, demonstrating their potential impact despite limited experience.
Mid-career insurance agent resume
This resume effectively showcases the applicant's strong sales performance and risk management expertise, demonstrating readiness for leadership roles. The consistent achievements in client satisfaction and policy growth reflect a proven track record of success, positioning them well for higher responsibilities.
Experienced insurance agent resume
The work history section effectively highlights the applicant's extensive experience in the insurance sector, showcasing a 40% annual increase in client portfolio and a 95% customer satisfaction rate. The use of bullet points improves readability, making it easy to quickly grasp key achievements.
Resume Template—Easy to Copy & Paste
David Nguyen
Detroit, MI 48204
(555)555-5555
david@example.com
Professional Summary
Dynamic Insurance Agent with 5 years of proven sales and risk assessment expertise. Expert at enhancing client portfolios and optimizing policy renewals using strategic techniques.
Work History
Insurance Agent
SecureLife Insurance Group - Detroit, MI
January 2023 - April 2026
- Increased client portfolio by 25%
- Exceeded sales targets by ,000 annually
- Improved policy renewal rates by 15%
Claims Specialist
GuardianAssure Insurance - Detroit, MI
January 2021 - December 2022
- Reduced claim processing time by 30%
- Resolved 200+ client issues monthly
- Optimized risk assessment protocols
Risk Management Advisor
SafeGuard Consulting - Detroit, MI
January 2019 - December 2020
- Analyzed risk scenarios for 100+ clients
- Saved businesses 200,000 annually
- Enhanced client strategic planning
Skills
- Client Relationship Management
- Sales Strategy
- Risk Assessment
- Policy Renewal Techniques
- Claims Processing
- Strategic Planning
- Portfolio Growth
- Market Analysis
Certifications
- Certified Insurance Counselor - The National Alliance
- Certified Financial Planner - CFP Board
Education
Master of Business Administration Finance
New York University Southgate, MI
June 2017
Bachelor of Arts Economics
City College of New York Southgate, MI
June 2015
Languages
- Spanish - C2
- Proficient - French
- B1 - Intermediate
- German - A2
- Elementary
How to Write an Insurance Agent Resume Summary
Your resume summary is the first opportunity to capture an employer's attention, so it’s important to make a lasting impression. As an insurance agent, you should highlight your strong communication skills and ability to build client relationships in this section. To illustrate effective resume summaries, we’ll provide examples that demonstrate best practices and common pitfalls in showcasing your qualifications:
I am an experienced insurance agent with a solid background in the industry. I hope to find a position that allows me to use my abilities and be part of a successful team. A company that values employee growth and offers good benefits would be great for me. I believe I can make a positive impact if given the chance.
- Lacks specific details about the job seeker’s achievements or expertise, making it vague
- Overuses personal language and fails to highlight skills relevant to potential employers
- Emphasizes what the job seeker seeks instead of showcasing how they can contribute to the organization
Results-driven insurance agent with over 7 years of experience in providing tailored insurance solutions to clients across various sectors. Achieved a 20% increase in client retention rates through personalized service and proactive policy reviews. Proficient in risk assessment, claims processing, and using CRM software to improve customer relationships and streamline operations.
- Begins with a clear indication of the applicant's experience level and industry expertise
- Highlights quantifiable achievements that reflect the agent's impact on client satisfaction and business growth
- Showcases relevant skills that are important for success in the insurance sector
Pro Tip
Showcasing Your Work Experience
The work experience section is the centerpiece of your resume as an insurance agent. This area will contain the bulk of your content, and good resume templates always emphasize its importance.
In this section, list your previous jobs in reverse-chronological order. Include three to four bullet points for each role, detailing your accomplishments and contributions in the insurance industry.
To craft a compelling work history section, we’ve prepared examples showcasing effective entries for insurance agents. These examples will illustrate what stands out and what should be avoided:
Insurance Agent
ABC Insurance Group – Los Angeles, CA
- Helped clients find insurance.
- Filled out forms and submitted claims.
- Communicated with customers in person and over the phone.
- Provided quotes based on client needs.
- Lacks specific details about achievements or metrics
- Bullet points are overly simplistic and fail to highlight skills
- Does not convey the impact made on clients or the company
Insurance Agent
Statewide Insurance Group – Orlando, FL
March 2020 - Present
- Develop customized insurance solutions for clients, resulting in a 30% increase in policy renewals year-over-year.
- Conduct thorough risk assessments to identify client needs, improving customer satisfaction ratings by 40%.
- Mentor junior agents in effective sales techniques and compliance standards, leading to improved team performance and client retention.
- Starts each bullet with compelling action verbs that highlight the applicant's contributions
- Incorporates specific metrics that demonstrate measurable success and impact on the business
- Showcases essential skills relevant to insurance sales and client relationship management
While your resume summary and work experience are important, it's essential not to overlook other sections that contribute to a strong application. Each part of your resume plays a role in showcasing your qualifications. For more detailed guidance, refer to our comprehensive guide on how to write a resume.
Top Skills to Include on Your Resume
Including a skills section on your resume is important for showcasing your professional capabilities to potential employers. This targeted area helps job seekers highlight specific competencies that align with the roles they are applying for, making their applications more compelling.
Hiring managers rely on this section to quickly evaluate whether applicants meet essential qualifications. It enables applicants to directly address job requirements, ensuring that insurance agent professionals present both hard and soft skills effectively, which will be discussed further below.
Soft skills are essential for insurance agents as they encompass traits like active listening and problem-solving, which foster trust and build strong client relationships.
When choosing skills for your resume, it’s important to align them with what employers expect. Many organizations use automated screening systems that filter out job seekers lacking essential resume skills.
To better understand which skills to highlight, take the time to review job postings carefully. Look for specific terms and requirements that can help you tailor your resume for both recruiters and ATS filters.
Pro Tip
10 skills that appear on successful insurance agent resumes
To capture the interest of recruiters, it’s important to highlight high-demand skills relevant to insurance agent roles. These essential skills are highlighted in resume examples, helping you apply confidently with a polished professional image.
By the way, here are 10 key skills that you should consider incorporating into your resume if they align with your experience and job requirements:
Customer service
Sales skill
Attention to detail
Analytical thinking
Negotiation skills
Knowledge of insurance laws and regulations
Problem-solving abilities
Time management
Effective communication
Team collaboration
Based on analysis of 5,000+ sales professional resumes from 2023-2024
Resume Format Examples
Choosing the right resume format is important for insurance agents, as it showcases key skills and experiences that align with industry demands, improving your chances of standing out to potential employers.
Functional
Focuses on skills rather than previous jobs
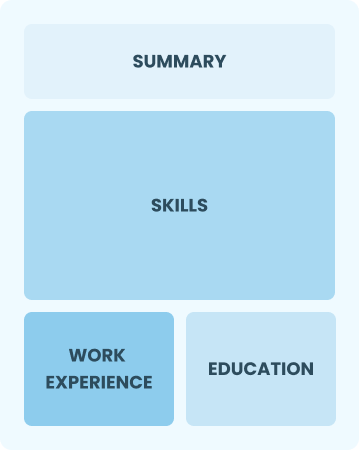
Best for:
Recent graduates and career changers with limited experience in insurance
Combination
Balances skills and work history equally
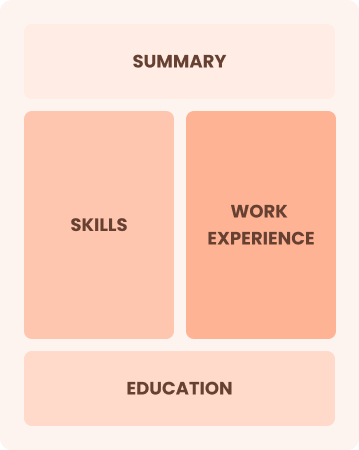
Best for:
Mid-career professionals eager to demonstrate their skills and seek new opportunities
Chronological
Emphasizes work history in reverse order

Best for:
Experienced agents excelling in complex policy solutions and client management
Frequently Asked Questions
Should I include a cover letter with my insurance agent resume?
Absolutely, including a cover letter can significantly improve your application by showcasing your personality and detailing your qualifications. It allows you to connect with the employer on a personal level and highlight why you're the perfect fit for the role. If you need assistance, consider using our guide on how to write a cover letter or try our easy-to-use Cover Letter Generator to craft an impressive letter quickly.
Can I use a resume if I’m applying internationally, or do I need a CV?
When applying for jobs abroad, use a CV rather than a resume, as many countries prefer this format. For guidance on how to write a CV that adheres to international standards, explore our comprehensive resources and CV examples, which detail formatting and essential content.
What soft skills are important for insurance agents?
Soft skills such as communication, empathy, and problem-solving are essential for insurance agents. These abilities foster trust and rapport with clients, allowing agents to better understand their needs and provide tailored solutions. Strong interpersonal skills improve collaboration within teams, leading to more effective service delivery.
I’m transitioning from another field. How should I highlight my experience?
Highlight your transferable skills, such as communication, customer service, and negotiation, gained from previous roles. These abilities showcase your potential value in the insurance industry, even if you're new to it. Use specific examples from past experiences to demonstrate how you've handled challenges relevant to an insurance agent's responsibilities.
How should I format a cover letter for an insurance agent job?
To format a cover letter, start with your contact details and include a formal greeting. Follow this by introducing yourself in an engaging way that emphasizes your interest in the insurance agent role. In the body, clearly outline how your skills and experiences relate to the job description. End with a strong closing statement that encourages further discussion.
Should I use a cover letter template?
Yes, using a cover letter template tailored for insurance agents can improve your application by providing a clear structure and helping you organize your content. This approach allows you to showcase relevant skills such as client relationship management and knowledge of policy regulations, making a strong impression on hiring managers.








