Hard skills encompass competencies like crisis intervention, behavioral assessment, and therapeutic communication. These skills are essential for behavioral health technicians to support patients.
Popular Behavioral Health Technician Resume Examples
Explore our top behavioral health technician resume examples that highlight valuable skills like crisis intervention, patient support, and effective communication. These samples can help you present your strengths and experiences to potential employers.
Want to craft an impressive resume? Our Resume Builder provides user-friendly templates tailored for professionals in the behavioral health field, making it easy to emphasize your qualifications.
Recommended
Entry-level behavioral health technician resume
This entry-level resume highlights the applicant's clinical skills and accomplishments in behavioral health, showcasing their experience in patient care and therapeutic interventions. New professionals need to demonstrate their knowledge of mental health practices and a commitment to improving patient outcomes through their resume, even with limited work experience.
Mid-career behavioral health technician resume
This resume effectively showcases the job seeker's significant achievements and skills in behavioral health, indicating their readiness for advanced roles. The progression from technician to leadership highlights a commitment to patient-centered care and innovative practices, essential for handling complex challenges in mental health settings.
Experienced behavioral health technician resume
The work history section highlights the applicant's extensive experience in behavioral health, showcasing key achievements such as a 20% reduction in patient relapse and a 35% increase in satisfaction rates. The bullet-point format allows for quick and easy scanning of their compelling contributions.
Resume Template—Easy to Copy & Paste
Yuki Miller
Portland, ME 04108
(555)555-5555
Yuki.Miller@example.com
Professional Summary
Dedicated Behavioral Health Technician with 5 years of experience. Skilled in patient-centered care, crisis intervention, and therapy facilitation. Proven track record in reducing relapse rates and improving recovery outcomes.
Work History
Behavioral Health Technician
Serenity Behavioral Solutions - Portland, ME
March 2024 - March 2026
- Provided mental health assistance to 75+ patients weekly.
- Implemented recovery plans, improving outcomes by 20%.
- Facilitated 50+ group therapy sessions for patient support.
Mental Health Support Specialist
Harmony HealthCare Center - Portland, ME
February 2022 - February 2024
- Coordinated care plans for 50+ patients monthly.
- Led crisis intervention reducing patient risks by 15%.
- Tracked client progress using in-depth electronic records.
Rehabilitation Counselor Assistant
Ridgeview Wellness Clinic - Westbrook, ME
March 2021 - January 2022
- Supported 30+ patients with addiction recovery programs.
- Conducted individual and group counseling sessions weekly.
- Assisted therapists, improving patient satisfaction by 18%.
Languages
- Spanish - Beginner (A1)
- French - Intermediate (B1)
- German - Beginner (A1)
Skills
- Mental health crisis intervention
- Patient-centered care
- Therapeutic communication
- Behavioral therapy techniques
- Group counseling facilitation
- Care plan development
- Electronic health records management
- Addiction recovery support
Certifications
- Certified Behavioral Health Technician (CBHT) - National Career Certification Board
- Mental Health First Aid Certification - National Council for Mental Wellbeing
Education
Master's Degree Clinical Psychology
Arizona State University Tempe, Arizona
May 2020
Bachelor's Degree Psychology
University of Arizona Tucson, Arizona
May 2018
How to Write a Behavioral Health Technician Resume Summary
Your resume summary is your chance to make a lasting impression on hiring managers. This section serves as the first glimpse employers get of your qualifications and passion for the role.
As a behavioral health technician, you should emphasize your interpersonal skills, empathy, and experience in supporting individuals with mental health challenges. Highlight any relevant training or certifications that showcase your readiness for this vital position.
To assist you further, we’ve included examples below that illustrate effective resume summaries and clarify what works well in this context:
I am a dedicated behavioral health technician with years of experience in the field. I want to find a position where I can apply my skills and help others. A job that offers good pay and benefits is what I'm looking for. I believe I would be a great addition to your team if given the chance.
- Lacks specific details about the job seeker’s achievements or skills relevant to behavioral health
- Overly focuses on personal desires rather than highlighting how they can contribute to the organization
- Uses generic phrases that do not effectively demonstrate their unique value in a competitive job market
Compassionate behavioral health technician with 4 years of experience in mental health settings, providing support to patients with a range of psychological disorders. Improved patient engagement by 30% through implementation of individualized therapy plans and group activities. Proficient in crisis intervention techniques, patient assessment, and maintaining accurate clinical documentation.
- Starts with specific years of experience and outlines the relevant work environment
- Highlights a quantifiable achievement that clearly demonstrates impact on patient care and engagement
- Enumerates key skills that are essential for the role, showing readiness to meet job demands
Pro Tip
Showcasing Your Work Experience
The work experience section is the focal point of your resume as a behavioral health technician, containing the bulk of your content. Resume templates always emphasize this important section.
Organize this portion in reverse-chronological order, detailing your previous positions. Use bullet points to highlight key achievements and responsibilities you’ve had in each role.
To further assist you, we'll present a couple of examples that illustrate what makes a strong work history for behavioral health technicians. These examples will clarify what works well and what should be avoided:
Behavioral Health Technician
Hope Mental Health Center – Los Angeles, CA
- Assisted patients with daily activities.
- Monitored patient behavior.
- Performed documentation tasks.
- Collaborated with healthcare staff.
- Lacks specifics about the nature of patient interactions
- Bullet points do not highlight any measurable outcomes or achievements
- Focuses on routine duties rather than showing impact on patient care
Behavioral Health Technician
Caring Minds Mental Health Services – Atlanta, GA
March 2020 - Present
- Assist in the daily care and supervision of patients with mental health conditions, ensuring a safe and supportive environment.
- Implement therapeutic activities tailored to individual patient needs, contributing to a 30% increase in engagement during group sessions.
- Document patient progress and collaborate with healthcare professionals to refine treatment plans, improving overall care quality.
- Starts each bullet point with compelling action verbs that clearly convey the applicant's contributions
- Incorporates specific metrics to illustrate tangible impacts on patient engagement and care quality
- Highlights relevant skills such as documentation and collaboration that are critical for success in behavioral health
While your resume summary and work experience typically take center stage, don't overlook the importance of other sections. Each part contributes to a compelling narrative about your qualifications. For more detailed insights on crafting an effective resume, explore our comprehensive guide on how to write a resume.
Top Skills to Include on Your Resume
A well-crafted skills section is a vital component of any resume, providing essential information that helps both job seekers and employers. This section allows applicants to succinctly showcase their qualifications and capabilities, making it easier for hiring managers to identify potential matches.
For employers, this area serves as a quick reference point to evaluate if applicants meet the necessary criteria for the role. Behavioral health technician professionals should emphasize both their technical skills and interpersonal qualities, which will be discussed further in the following sections.
Soft skills are important for behavioral health technicians, with qualities like patience, active listening, and emotional intelligence helping to foster trust and support in their interactions with patients.
When selecting skills for your resume, it's essential to align them with what employers expect. Many organizations rely on automated screening systems to filter job seekers based on these important resume skills.
To tailor your application, review job postings for insights into the specific skills that recruiters seek. This practice ensures you highlight relevant abilities that resonate with both hiring managers and ATS algorithms.
Pro Tip
10 skills that appear on successful behavioral health technician resumes
Improve your resume to grab the attention of recruiters by highlighting sought-after skills for behavioral health technicians. These valuable skills can be seen in our resume examples, equipping you with the confidence needed to pursue job opportunities.
Here are 10 essential skills you should consider including in your resume if they align with your experience and job requirements:
Empathy
Active listening
Crisis intervention
Behavioral observation
Team collaboration
Documentation skill
Patient care techniques
Conflict resolution
Time management
Cultural competence
Based on analysis of 5,000+ health care support professional resumes from 2023-2024
Resume Format Examples
Selecting the appropriate resume format is important for behavioral health technicians as it showcases your key skills, relevant experience, and professional development in a clear and organized manner.
Functional
Focuses on skills rather than previous jobs
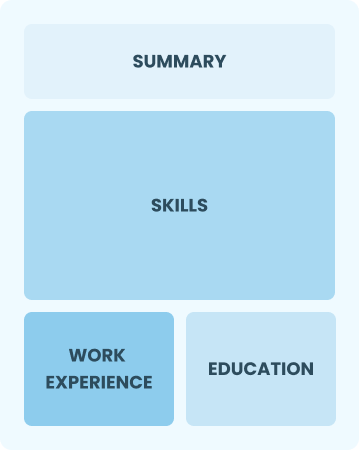
Best for:
Recent graduates and career changers with limited experience in the field
Combination
Balances skills and work history equally
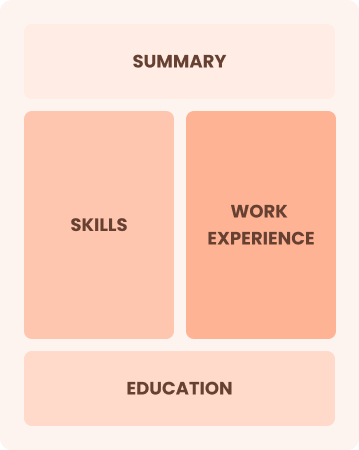
Best for:
Mid-career professionals eager to highlight their skills and demonstrate growth potential
Chronological
Emphasizes work history in reverse order

Best for:
Experts leading innovative treatment programs in mental health
Frequently Asked Questions
Should I include a cover letter with my behavioral health technician resume?
Absolutely. Including a cover letter is a great way to improve your application and showcase your enthusiasm for the position. It allows you to highlight specific experiences that align with the job requirements. For tips on crafting an effective cover letter, consider checking out our comprehensive guide on how to write a cover letter or use our Cover Letter Generator for quick assistance.
Can I use a resume if I’m applying internationally, or do I need a CV?
When applying internationally, use a CV instead of a resume to showcase your full academic and professional history. For guidance on how to write a CV, explore our templates and resources designed to help job seekers format and create effective CVs that meet the expectations of employers abroad. Additionally, you can view various CV examples for further inspiration and understanding.
What soft skills are important for behavioral health technicians?
Soft skills like compassion, active listening, and adaptability, are essential for behavioral health technicians. These interpersonal skills foster trust with patients and improve teamwork with colleagues, ensuring a supportive environment that promotes recovery and effective communication within the healthcare setting.
I’m transitioning from another field. How should I highlight my experience?
When transitioning to a behavioral health technician role, highlight your transferable skills like communication, empathy, and teamwork. These abilities illustrate your potential impact on patient care, even if your background isn’t directly in healthcare. Share concrete examples from previous jobs that showcase how you handled challenges or supported others, making a strong case for your candidacy.
Where can I find inspiration for writing my cover letter as a behavioral health technician?
If you're seeking inspiration for your cover letter as a behavioral health technician, explore our expertly crafted cover letter examples. These samples provide valuable content ideas, formatting tips, and effective ways to showcase your qualifications, helping you stand out in your job applications.
Should I include a personal mission statement on my behavioral health technician resume?
Including a personal mission statement on your resume is highly recommended. It showcases your commitment to behavioral health and aligns with organizations that prioritize patient-centered care and community support. This approach resonates well with mission-driven companies seeking job seekers who share their values.







