Hard skills include expertise in chemotherapy administration, symptom management, and patient education that oncology nurses must demonstrate to ensure comprehensive cancer care.
Popular Oncology Nurse Resume Examples
Discover our top oncology nurse resume examples that emphasize critical skills such as patient advocacy, treatment administration, and empathetic communication. These templates illustrate how to showcase your accomplishments in a competitive job market.
Ready to design your standout resume? Our Resume Builder offers user-friendly templates specifically crafted for healthcare professionals, making it simpler to highlight your expertise and attract potential employers.
Recommended
Entry-level oncology nurse resume
This entry-level resume for an oncology nurse highlights the applicant's strong clinical skills and compelling contributions during their nursing education and early career. New professionals in this field must showcase their competencies in patient care and specialized knowledge to attract employer interest, even with limited direct work experience.
Mid-career oncology nurse resume
This resume effectively showcases the job seeker's extensive oncology experience and leadership capabilities, emphasizing their proactive approach to patient care and operational improvements. The demonstrated ability to train peers and implement quality initiatives indicates a strong readiness for advanced roles in healthcare.
Experienced oncology nurse resume
This work history section highlights the applicant's extensive experience as an oncology nurse, showcasing a 20% improvement in patient recovery rates and overseeing over 100 chemotherapy treatments. The clear bullet point format improves readability, making accomplishments easy to identify for hiring managers.
Resume Template—Easy to Copy & Paste
Aya Wang
Riverside, CA 92516
(555)555-5555
aya@example.com
Professional Summary
Experienced oncology nurse specializing in chemotherapy and symptom management. Proven track record of improving patient satisfaction by 20% while managing a high-volume caseload. Skilled in team collaboration and patient education.
Work History
Oncology Nurse
Greenfield Hospital - Riverside, CA
April 2023 - April 2026
- Managed 100+ chemotherapy regimens monthly.
- Improved patient satisfaction by 20% annually.
- Collaborated with 15 oncologists for patient care.
Hematology Nurse
Riverside Medical Group - Riverside, CA
April 2020 - March 2023
- Assisted in 250+ bone marrow biopsies annually.
- Reduced patient waiting times by 30%.
- Coordinated blood transfusions for 50 patients weekly.
Registered Nurse
Harmony Health Center - Los Angeles, CA
April 2018 - March 2020
- Monitored vitals for 30 patients daily.
- Decreased medication errors by 15%.
- Educated patients on post-discharge care.
Skills
- Chemotherapy Administration
- Patient Assessment
- Clinical Documentation
- Symptom Management
- Patient Education
- Critical Care Nursing
- IV Therapy
- Team Collaboration
Certifications
- Oncology Certified Nurse - Oncology Nursing Certification Corporation
- Advanced Cardiac Life Support (ACLS) - American Heart Association
Education
Master of Science in Nursing Oncology Nursing
University of Washington Sunnydale, CA
June 2018
Bachelor of Science in Nursing Nursing
Seattle University Sunnydale, CA
June 2016
Languages
- Spanish - C2
- Proficient - French
- B1 - Intermediate
- Mandarin - A2
- Elementary
How to Write a Oncology Nurse Resume Summary
Your resume summary is the first opportunity to captivate hiring managers, making it essential to clearly convey your qualifications. As an oncology nurse, you should emphasize your specialized knowledge and compassionate patient care skills that set you apart in this challenging field. To illustrate effective strategies for crafting a compelling summary, let's explore examples that highlight both strong and weak approaches:
I am an experienced oncology nurse with a background in patient care and treatment protocols. I hope to find a position that allows me to use my skills effectively and contribute positively to the healthcare team. A supportive work environment with good hours is very important to me, and I believe I can help improve patient outcomes if given the chance.
- Lacks specific examples of nursing skills or accomplishments relevant to oncology
- Focuses on personal needs rather than emphasizing how the applicant can benefit the employer or patients
- Uses generic phrases that do not convey genuine enthusiasm or expertise in oncology nursing
Compassionate oncology nurse with 7+ years of experience managing complex cancer care in both inpatient and outpatient settings. Successfully improved patient satisfaction scores by 20% through the implementation of personalized care plans and regular follow-up protocols. Proficient in chemotherapy administration, symptom management, and using electronic health records to improve patient safety and communication.
- Begins with specific experience duration and specialty focus relevant to oncology nursing
- Highlights a quantifiable achievement that reflects direct impact on patient satisfaction and care quality
- Showcases relevant technical skills that align with the demands of oncology nursing roles
Pro Tip
Showcasing Your Work Experience
As an oncology nurse, the work experience section of your resume is where you'll capture the essence of your career. This core area should be a focal point, and using high-quality resume templates will ensure this section stands out.
Organize your past roles in reverse-chronological order, with bullet points to highlight significant achievements and patient care accomplishments specific to oncology nursing.
To provide clarity, we’ll present a couple of examples illustrating effective entries for oncology nurses. These examples will help you discern what makes a strong impression and what doesn’t:
Oncology Nurse
City Hospital – New York, NY
- Provided care to cancer patients.
- Maintained patient records and documentation.
- Collaborated with healthcare teams.
- Administered treatments and medications as required.
- Lacks specific employment dates for context
- Bullet points are overly simplistic and do not highlight unique skills or achievements
- Emphasizes routine duties rather than strong contributions or results
Oncology Nurse
City Hospital – Los Angeles, CA
March 2020 - Present
- Administer chemotherapy and manage side effects for a patient caseload of 15+, ensuring optimal comfort and care.
- Develop and implement patient education programs on treatment options, leading to a 30% increase in patient understanding and adherence.
- Coordinate with oncologists and support staff to improve multidisciplinary approaches, resulting in improved patient satisfaction scores.
- Starts each bullet with dynamic action verbs that clearly convey the nurse’s contributions
- Incorporates specific metrics to highlight the impact of initiatives on patient care and outcomes
- Demonstrates relevant skills such as communication, teamwork, and patient advocacy throughout the accomplishments
While your resume summary and work experience are important, don’t overlook the significance of other sections. Each part of your resume contributes to showcasing your qualifications. For detailed insights on formatting these sections, refer to our comprehensive guide on how to write a resume.
Top Skills to Include on Your Resume
Including a skills section on your resume is vital as it provides a clear snapshot of your qualifications. This helps job seekers effectively communicate their strengths while allowing employers to quickly gauge potential fit for the role.
Hiring managers rely on this section to swiftly evaluate whether applicants meet essential criteria, streamlining the hiring process. Oncology nurse professionals should highlight both technical and interpersonal skills that illustrate their expertise in patient care and collaboration, which will be discussed further below.
Soft skills are essential for oncology nurses, as they foster trust and understanding with patients. This improves care quality and supports emotional well-being during treatment journeys.
Choosing the right resume skills is important for standing out in your job application. Many employers use automated systems to filter job seekers, so aligning your skills with their expectations can significantly improve your chances of making it through the initial screening.
To highlight your abilities well, take time to analyze job postings relevant to your desired position. These listings often provide insights into which competencies are most valued by recruiters and can help you tailor your resume accordingly.
Pro Tip
10 skills that appear on successful oncology nurse resumes
Showcasing essential skills in your resume is key to catching the eye of recruiters searching for oncology nurses. Our resume examples highlight these sought-after abilities, enabling you to present yourself with confidence and professionalism.
By the way, consider incorporating relevant skills from the following list that match your experience and job requirements:
Patient assessment
Chemotherapy administration
Pain management
Communication
Team collaboration
Knowledge of cancer treatments
Emotional support for patients and families
Time management
Attention to detail
Clinical documentation
Based on analysis of 5,000+ nursing professional resumes from 2023-2024
Resume Format Examples
Choosing the correct resume format is important for oncology nurses to showcase their specialized skills, clinical experience, and career growth clearly and strongly.
Functional
Focuses on skills rather than previous jobs
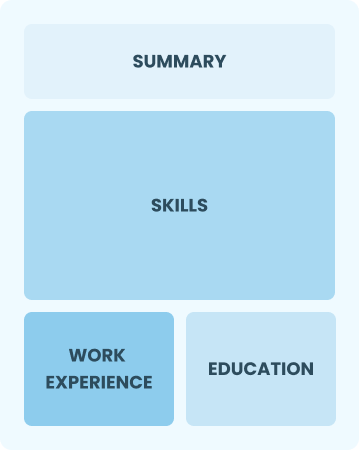
Best for:
Best for recent graduates and career changers with up to two years of experience
Combination
Balances skills and work history equally
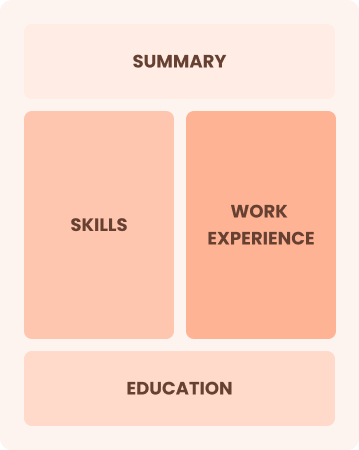
Best for:
Mid-career professionals focused on demonstrating their skills and growth potential
Chronological
Emphasizes work history in reverse order

Best for:
Experienced leaders in cancer care and treatment innovation
Frequently Asked Questions
Should I include a cover letter with my oncology nurse resume?
Absolutely, including a cover letter can significantly improve your application by showcasing your enthusiasm and detailing relevant experiences. A well-crafted cover letter helps you connect with recruiters on a personal level. For tips and templates, visit our comprehensive guide on how to write a cover letter or use our Cover Letter Generator to create one effortlessly.
Can I use a resume if I’m applying internationally, or do I need a CV?
When applying for jobs outside the U.S., use a CV instead of a resume, as many countries prefer this format. To assist you, we offer CV examples to guide you in crafting an effective CV that aligns with international standards. For more detailed guidance, explore our resources on how to write a CV, ensuring your application stands out globally.
What soft skills are important for oncology nurses?
Soft skills like empathy, active listening, and interpersonal skills such as effective communication are important for oncology nurses. These abilities foster trust with patients and improve collaboration with healthcare teams. Building strong relationships through these skills can significantly improve patient care and overall treatment experiences.
I’m transitioning from another field. How should I highlight my experience?
Highlight your transferable skills, such as communication, empathy, and teamwork, when applying for oncology nurse roles. Even if your experience in healthcare is limited, these attributes are essential in patient care. Share concrete examples from your past work that illustrate how you've supported others or managed challenging situations to showcase your readiness for this important role.
How should I format a cover letter for a oncology nurse job?
To format a cover letter for oncology nurse positions, start with your contact details and a professional salutation. Include an engaging introduction to highlight your passion for nursing. In the body, clearly outline your relevant qualifications and experiences. Tailor each section to reflect the specific job requirements, and finish with a compelling call to action inviting further discussion.
Should I use a cover letter template?
Yes, using a cover letter template specifically tailored for oncology nursing can improve your ability to present critical skills such as patient care expertise and knowledge of cancer treatments. This structured approach ensures you organize your experiences and achievements well, making a strong impression on hiring managers.








